Why Your Back Pain Keeps Coming Back (And How to Break the Cycle)

If your back pain keeps returning despite rest, stretching, or the occasional physio visit, the problem isn't your pain tolerance - it's that the root cause was never fully addressed. Recurring back pain is one of the most common health complaints in the world, and most people spend years managing the symptoms rather than fixing the underlying imbalance driving them.
TL;DR
- Recurring back pain is usually caused by unresolved muscle imbalances, not a single injury
- Rest alone does not fix the structural causes – it only reduces flare-up symptoms
- The pain cycle is maintained by weak stabilizers, tight compensating muscles, and poor movement habits
- Desk workers, parents, and aging adults are at highest risk
- A personalized, progressive approach breaks the cycle – generic advice rarely does
What Is Recurring Back Pain?
Recurring back pain is a pattern of repeated musculoskeletal flare-ups caused by unresolved structural imbalances, where temporary symptom relief is mistaken for full recovery.
This is the key distinction most people miss. The pain going away does not mean the problem is solved. It means the tissue irritation has settled enough to stop signaling – but the underlying weakness, tightness, or misalignment that caused it is still there, waiting for the next trigger.
For most adults, recurring back pain falls into two categories:
- Lower back pain – driven by weak glutes and core, tight hip flexors, or lumbar instability
- Upper and mid-back pain – driven by rounded shoulders, forward head posture, and thoracic stiffness from prolonged sitting
Many people experience both simultaneously.
Why Does Back Pain Keep Coming Back?
The answer is almost always one of these five root causes – and most flare-ups involve more than one at the same time.
1. The Pain Was Treated, Not the Cause
Rest, painkillers, heat packs, and even many physiotherapy sessions focus on reducing pain and inflammation. They work – in the short term. But if the muscle imbalance or movement pattern that created the pain is still present when you return to normal activity, the cycle restarts within weeks.
Posture specialists suggest that symptom-focused treatment without corrective rehabilitation is the single biggest reason back pain becomes chronic.
2. Weak Deep Core Stabilizers
The deep core – specifically the transverse abdominis, multifidus, and pelvic floor – is the primary support system for the lumbar spine. These muscles don't show up in a six-pack, but they hold your spine stable during every movement you make.
Research in musculoskeletal rehab shows that people with chronic lower back pain consistently show delayed or reduced activation of these stabilizing muscles compared to pain-free individuals. The superficial muscles compensate – which leads to overload, fatigue, and re-injury.
3. Tight Hip Flexors and a Tilted Pelvis
Sitting for long periods shortens the hip flexor muscles at the front of the hips. When hip flexors are chronically tight, they pull the pelvis into an anterior tilt – an exaggerated lower back arch. This compresses the lumbar facet joints and puts the entire lower back under constant strain, even when you're standing still.
4. Inhibited Glutes
Prolonged sitting doesn't just shorten the hip flexors – it switches off the glutes. The gluteus maximus is the largest and most powerful muscle in the body, and a primary stabilizer of the pelvis and lower back. When it's not firing properly, the lower back compensates by absorbing loads the glutes should be handling.
Physiotherapists often refer to this as gluteal amnesia – and it's extremely common in desk workers, drivers, and anyone who sits for more than 6 hours a day.
5. Poor Movement Habits That Reload the Injury
Even after tissue healing and some strengthening, most people return to the same posture and movement patterns that caused the problem. The same desk setup, the same way of bending to pick things up, the same hours of unbroken sitting. Without changing the input, the output stays the same.
💡 Key Insight: Back pain doesn't come back because you're unlucky. It comes back because the structural conditions that caused it – weak stabilizers, tight hip flexors, inhibited glutes, poor movement habits – were never addressed. The pain was managed. The problem wasn't.
How Does the Pain Cycle Actually Work?
Understanding the mechanism helps you break it.
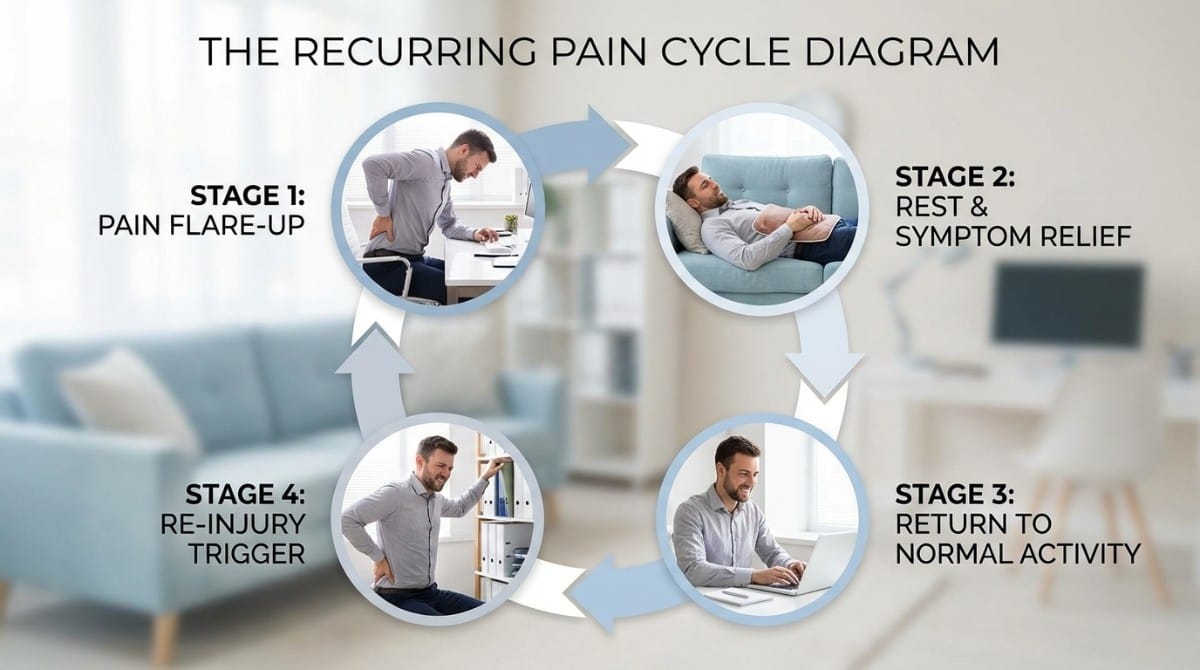
Here's how most recurring back pain cycles unfold:
- Trigger event – A movement, lift, or sustained posture irritates already-vulnerable tissue
- Acute pain phase – Inflammation and muscle guarding create sharp or aching pain
- Rest and passive treatment – Symptoms reduce over 3-10 days
- False recovery – Pain is gone, but the stabilizers are weaker and the imbalances are unchanged
- Return to normal activity – The same patterns reload the vulnerable structures
- Re-injury – Often from something minor – reaching, twisting, or a long car ride
The cycle typically shortens over time. Early episodes might be months apart. After years, the gap between flare-ups can compress to weeks.

What Happens If Recurring Back Pain Is Left Untreated?
Recurring back pain is not just inconvenient – it has a documented progression if the root causes aren't resolved.
- Tissue adaptation – Muscles and connective tissue adapt to their shortened or weakened state, making correction progressively harder
- Nerve sensitization – The nervous system can become hypersensitized to pain signals, meaning less stimulus triggers more pain over time
- Disc degeneration – Uneven spinal loading accelerates wear on intervertebral discs, increasing herniation risk
- Compensation injuries – As the lower back is protected, other areas (hips, knees, neck) absorb more load and develop their own problems
- Psychological impact – Chronic pain has well-documented links to anxiety, disrupted sleep, and reduced quality of life
Research in musculoskeletal rehab shows that untreated recurring back pain is one of the leading causes of long-term disability in working adults globally.
The Step-by-Step Recovery Framework: Breaking the Cycle
This is not a generic exercise list. It is a sequenced protocol that addresses the root causes in the right order.
Step 1 – Reduce Current Irritation (Days 1-3)
If you are in an active flare-up, the first priority is calming the tissue – not stretching aggressively or loading through pain.
- Apply gentle heat to the lower back for 15-20 minutes
- Perform Child's Pose (3 rounds of 5 slow breaths) to decompress the lumbar spine
- Walk for 10-15 minutes at a slow, comfortable pace – gentle movement is better than full rest
- Avoid: prolonged sitting, heavy lifting, and forward flexion under load
Step 2 – Release Tight Structures (Days 3-10)
Once acute pain has settled, begin releasing the tight muscles maintaining the imbalance.
- Hip Flexor Lunge Stretch – Step into a lunge, drop back knee to the floor, tuck tailbone slightly, reach arms overhead. Hold 30 seconds per side, 3 rounds. Directly targets shortened hip flexors driving anterior pelvic tilt.
- Thoracic Spine Rotation – Lie on your side, knees bent at 90 degrees. Reach the top arm across and let it fall to the opposite side. 8-10 slow repetitions per side. Restores mid-back mobility lost from desk posture.
- Piriformis Stretch – Lie on your back. Cross one ankle over the opposite knee. Draw both legs toward your chest. Hold 30-40 seconds per side. Releases the deep glute and hip rotators commonly tight in people with lower back pain.
- Child's Pose – Continue daily. 5 deep breaths, 3 rounds, morning and night.

Step 3 – Reactivate Inhibited Muscles (Days 7-21)
With tight structures releasing, the inhibited muscles need to be switched back on – particularly the glutes and deep core stabilizers.
- Glute Bridge – Lie on your back, feet flat, hip-width apart. Drive hips up until body forms a straight line from knees to shoulders. Squeeze glutes hard at the top for 2 seconds. Lower slowly. 3 sets of 15 reps. This is the single most important exercise for most recurring lower back pain sufferers.
- Dead Bug – Lie on your back, arms toward ceiling, knees at 90 degrees. Slowly lower one arm and the opposite leg toward the floor while maintaining a flat lower back. Return and switch sides. 3 sets of 8 per side. Activates deep core stabilizers without loading the spine.
- Bird Dog – On all fours, extend one arm and the opposite leg simultaneously. Hold 3 seconds. Return and switch. 3 sets of 10 per side. Trains the multifidus and transverse abdominis – the deep spinal stabilizers most disabled in chronic back pain.
- Clamshell – Lie on your side, knees bent, feet together. Rotate the top knee open like a clamshell without moving the pelvis. 3 sets of 15 per side. Reactivates gluteus medius, critical for pelvic stability during walking and standing.

Step 4 – Build Spinal Load Tolerance (Days 14-30)
Reactivated muscles need progressive loading to become reliable under the demands of real life.
- High Plank – Arms straight, wrists under shoulders, spine neutral. Hold for 10-20 deep breaths. 3-5 rounds. Integrates all core stabilizers under simultaneous demand.
- Romanian Deadlift (bodyweight or light load) – Hinge at the hips, soft knee bend, back flat, drive hips back until a hamstring stretch is felt. Drive hips forward to return. 3 sets of 10. Teaches correct hip hinge mechanics that protect the lower back during lifting.
- Wall Sit – Back flat against wall, thighs parallel to floor. Hold for 30-45 seconds, 3 rounds. Builds quadriceps and glute endurance needed to reduce lower back compensation during prolonged standing.
- Isometric Row (seated or standing) – Drive elbows back hard, squeeze shoulder blades together. Hold 10 seconds. Repeat every 1-2 hours. Maintains upper back activation throughout the workday.
Step 5 – Change the Daily Inputs (Ongoing)
No exercise program will hold if you return to the same environment and habits that caused the problem.
- Set a movement break alarm every 30 minutes during desk work
- Each alarm: stand, perform 10 glute squeezes, do 30 seconds of Standing Cat-Cow
- Check phone at eye level, not tilted down
- When lifting anything from the floor: hip hinge, not spinal flex
- When sitting: feet flat, knees at 90 degrees, lower back lightly supported
Best Exercises to Break the Recurring Back Pain Cycle (Quick List)
- Glute Bridge – Reactivates the primary lower back stabilizer. 3 sets of 15.
- Dead Bug – Activates deep core without spinal loading. 3 sets of 8 per side.
- Bird Dog – Trains multifidus and transverse abdominis directly. 3 sets of 10 per side.
- Hip Flexor Lunge Stretch – Releases the tightest driver of lower back strain. Daily.
- Piriformis Stretch – Releases deep hip tension compressing the lower back. Daily.
- High Plank – Integrates full core stability under load. 3-5 rounds.
- Child's Pose – Decompresses the lumbar spine and resets baseline. Morning and night.
- Thoracic Spine Rotation – Restores mid-back mobility. Daily.
Recurring Back Pain Recovery Timeline
| Phase | Focus | Expected Outcome |
|---|---|---|
| Days 1--3 | Reduce irritation | Acute pain settles, movement becomes easier |
| Days 3--10 | Release tight structures | Less stiffness, improved hip and thoracic mobility |
| Days 7--21 | Reactivate stabilizers | Glutes and deep core engaging, back feeling more supported |
| Days 14--30 | Build load tolerance | More confidence in movement, fewer compensation patterns |
| Ongoing | Habit change | Longer gaps between flare-ups, eventually no recurrence |
When This Approach Does Not Work
This protocol is effective for the majority of non-specific recurring lower back pain. However, it is not appropriate for all cases.
Seek clinical assessment before starting if you have:
- Radiating pain into the leg (sciatica) – may indicate nerve compression requiring specific treatment
- Bladder or bowel changes alongside back pain – requires urgent medical review
- Night pain that wakes you from sleep – may indicate non-mechanical causes requiring investigation
- A known disc herniation or spinal stenosis diagnosis – certain exercises can aggravate these conditions without professional guidance
- Pain that consistently worsens with exercise – a signal that tissue irritation needs to settle first
If any of the exercises in Step 3 or Step 4 increase your symptoms, stop and consult a physiotherapist before progressing.
Research & Expert Insight
- Research in musculoskeletal rehab consistently identifies weak deep stabilizers – specifically the multifidus and transverse abdominis – as a primary factor in recurrent lower back pain. These muscles show measurably reduced activation in people with chronic pain compared to pain-free controls.
- Posture specialists suggest that gluteal inhibition from prolonged sitting is one of the most underdiagnosed contributors to lower back instability in desk-working adults.
- Physiotherapists often recommend progressive motor retraining – not passive therapy – as the most evidence-supported long-term approach to breaking the recurring back pain cycle.
- Research in spinal biomechanics shows that anterior pelvic tilt increases lumbar compressive loading by a clinically significant margin – making hip flexor release a non-negotiable part of any lower back rehabilitation program.
Final Takeaway
Recurring back pain is not inevitable and it is not random. It follows a predictable cycle driven by identifiable structural causes. Rest breaks the flare-up but not the cycle. The only way to genuinely break it is to address all five root causes in sequence: reduce irritation, release tight structures, reactivate inhibited muscles, build load tolerance, and change the daily inputs driving the imbalance.
Follow the step-by-step framework consistently for 30 days. Most people notice a meaningful reduction in both frequency and intensity of flare-ups by the end of week two. After 30 days, many experience the longest pain-free stretch they have had in years.
Why Most Back Pain Programs Fail to Break the Cycle
The uncomfortable truth is that most approaches to recurring back pain – YouTube routines, generic NHS advice sheets, single physio visits – are not designed to break the cycle. They're designed to manage the current episode.
Three structural reasons they fail long-term:
- No personalization. Your pain is driven by your specific combination of tight muscles, weak stabilizers, and movement patterns. A program built for someone else will target the wrong things at the wrong intensity – and may skip the root cause entirely.
- No form feedback. Exercises like Bird Dog and Dead Bug require precise technique to activate the right muscles. Without feedback, most people perform them incorrectly and reinforce the compensation patterns they're trying to fix.
- No progression. As stabilizers strengthen, the program must advance to maintain adaptation. Static routines plateau within weeks – leaving your back under-supported just as activity levels return to normal.
The Smarter Approach: Backed AI 📱
Backed AI is an AI-powered posture correction and back pain relief app that addresses all three problems in one place.
- AI posture analysis scans your alignment using your phone camera – identifying the specific imbalances driving your pain, not a generic guess
- Personalized corrective programs are built around your scan and updated as you progress, ensuring the right exercises at the right stage
- Smart habit reminders keep your movement breaks and daily routines consistent – replacing willpower with structure
Ready to stop repeating the cycle? Backed AI gives you a clear, personalized path to recovery – built around your body, not someone else's average.
Download Backed AI and start correcting your posture today: backedapp.com
Frequently Asked Questions
Q1: Why does my back pain keep coming back even after it heals?
Because pain going away is not the same as the problem being solved. The muscle imbalances, weak stabilizers, and tight hip flexors that caused the pain are still present after tissue irritation settles. Until those are corrected, the same triggers will produce the same result.
Q2: What muscles are responsible for recurring lower back pain?
The most commonly implicated muscles are weak deep core stabilizers (multifidus, transverse abdominis), inhibited glutes, and overly tight hip flexors. Addressing all three in sequence is essential for lasting recovery.
Q3: Is it better to rest or exercise when back pain returns?
Gentle movement is generally better than full rest for most non-acute back pain. Light walking, Child's Pose, and gentle hip stretches help reduce inflammation and prevent the stiffness that often worsens pain after complete rest.
Q4: How long does it take to break the recurring back pain cycle?
Most people notice fewer and less severe flare-ups within 3-4 weeks of consistent corrective exercise. A full structural improvement – where the stabilizers are strong enough to protect the spine under load – typically takes 8-12 weeks of progressive training.
Q5: Can an app really help with chronic back pain?
Yes – particularly apps like Backed AI that combine AI posture scanning with personalized corrective programs. The personalization component is critical: generic exercises often miss the specific imbalance driving an individual's pain. An AI-assessed program targets the actual root cause rather than a statistical average.


