Why Does My Lower Back Hurt When I Stand for a Long Time?

Lower back pain when standing is almost always caused by increased spinal load, poor posture patterns, or muscle fatigue - and it's almost always fixable. The pain is your body signalling that something in your alignment or strength foundation isn't holding up under gravity. Understanding the specific cause is what separates a real fix from temporary relief.
TL;DR:
- Standing increases compressive load on the lumbar spine, which tires muscles and stresses joints
- Poor posture - especially anterior pelvic tilt or flat back - dramatically worsens standing pain
- Weak glutes and core force the lower back to carry load it wasn't designed to handle alone
- Most standing-related lower back pain responds well to targeted strengthening and posture correction
- Stretching alone rarely solves it - muscle activation and alignment correction are the real fix
- Backed AI can identify your specific postural pattern and build a personalised corrective plan
What Is Lower Back Pain When Standing?
Lower back pain when standing is lumbar discomfort that develops or worsens after remaining upright for extended periods, typically caused by spinal loading, postural misalignment, or insufficient muscular support.
Most people assume that standing is "neutral" - that it shouldn't hurt. But standing is actually an active, demanding task for your spine. Your lumbar vertebrae, discs, joints, and surrounding muscles are all working constantly to keep you upright against gravity. When that system is unbalanced, pain builds over time.
The pattern is recognisable: you're fine for the first 10-15 minutes, then a dull ache starts building in the lower back. You shift your weight, lean on something, or walk a few steps to get relief. The pain returns the moment you stand still again.
This isn't random. It's a signal - and it has a source.
Why Does the Lower Back Hurt More When You Stand Still?
There's a reason walking often feels better than standing in one spot. Movement distributes load across changing muscle groups. Standing still locks the same structures under continuous pressure.
Here's what's happening in your lower back when you stand:
- Your lumbar discs compress under the weight of your upper body
- The small facet joints at the back of each vertebra take on sustained load
- Your lower back muscles - the erector spinae - contract continuously to prevent forward collapse
- If your posture tilts even slightly, these forces multiply in specific areas
Physiotherapists often explain it this way: standing is like holding a weight at arm's length. Even a light weight becomes painful over time. Your lower back muscles face the same challenge when posture is off.
Research in musculoskeletal health shows that simply standing for two hours can induce temporary lower back pain in up to 50% of otherwise healthy adults due to progressive back muscle fatigue. For people with underlying postural imbalances, this threshold is far lower.
What Causes Lower Back Pain When Standing?
Not all standing-related back pain has the same root cause. These are the most common drivers - and they often overlap.
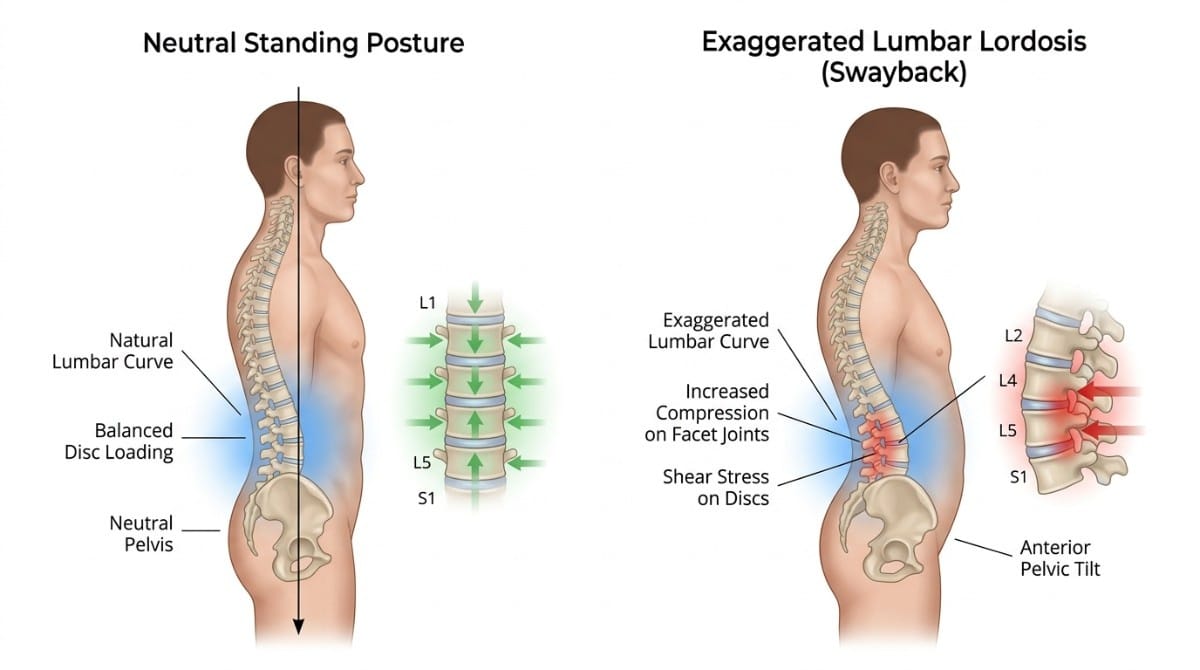
1. Poor Posture and Anterior Pelvic Tilt
This is the most common driver of standing back pain in desk workers and active adults under 60.
When the pelvis tilts forward (anterior pelvic tilt), it exaggerates the lower back's natural curve (lordosis). This compresses the facet joints at the back of the spine and chronically tightens the lumbar muscles.
The result: a deep, aching lower back pain that builds the longer you stand and eases when you sit or flex forward.
2. Weak Glutes and Core
Your glutes and deep core are designed to share the spinal load when you stand. When they're weak - which is extremely common after prolonged sitting - your lower back picks up that load alone.
Weak posterior chain = overloaded lower back. This is one of the most underappreciated causes of standing back pain, and it's entirely correctable with the right exercises.
3. Tight Hip Flexors
Tight hip flexors pull the front of the pelvis downward, forcing the lower back into an exaggerated arch. They also limit hip extension, which means each step you take shifts more demand onto the lumbar spine.
4. Flat Back Posture
The opposite of anterior pelvic tilt. Here, the lumbar curve flattens, shifting your center of gravity forward. Your lower back muscles fatigue faster trying to hold you upright, and the discs carry load unevenly.
5. Lumbar Muscle Fatigue
Sometimes it's simply endurance. If your lower back muscles aren't conditioned for prolonged upright activity, they fatigue and ache - similar to how any untrained muscle behaves under sustained use.
🔑 Key Insight: Lower back pain when standing is almost always a symptom, not a diagnosis. The source could be postural, muscular, or structural - and targeting the wrong one means getting the wrong result. Identifying your specific pattern matters more than picking any exercise.
Best Exercises for Lower Back Pain When Standing (Quick List)
These exercises address the most common muscular and postural causes. Do them consistently - not just on painful days.
- Glute Bridge - Activates and strengthens the glutes to reduce lumbar loading during standing. 3 sets of 12 reps. Hold 2 seconds at the top.
- Hip Flexor Lunge Stretch - Releases tight hip flexors that are tilting the pelvis and compressing the lower back. 30 seconds each side, twice daily.
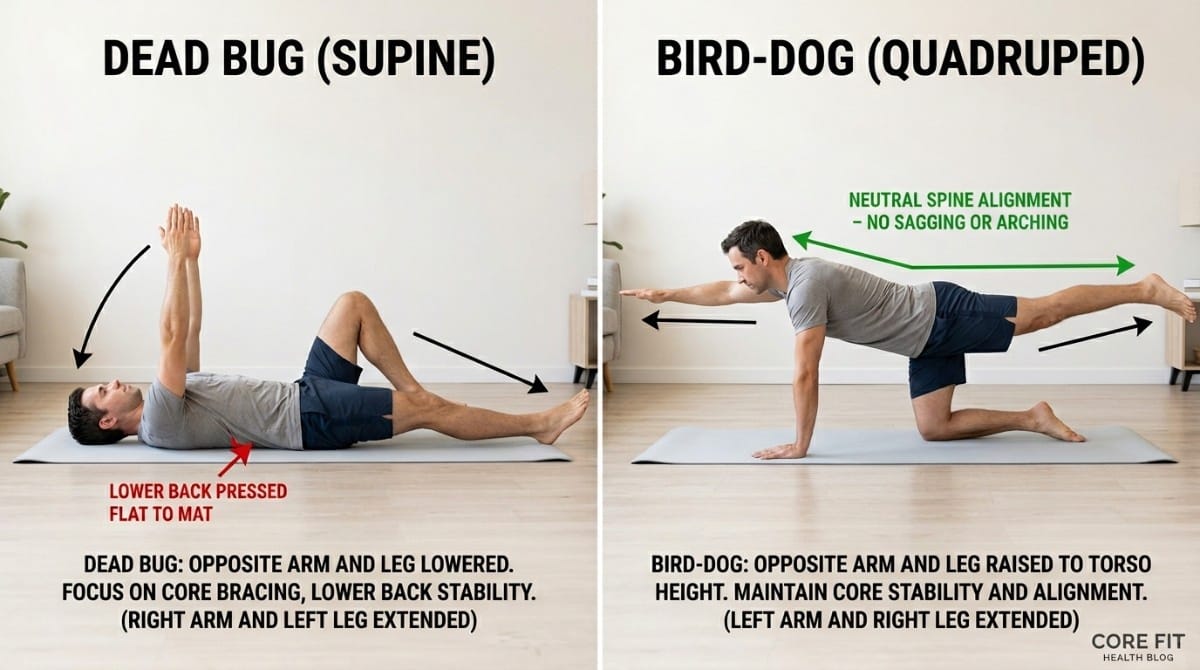
- Dead Bug - Builds deep core stability without loading the lumbar spine. 3 sets of 8 per side. Keep lower back pressed into the floor.
- Bird-Dog - Trains the posterior chain and spinal stabilisers together. 3 sets of 8 per side. Move slowly and controlled.
- Cat-Cow Mobilisation - Restores lumbar mobility and reduces joint stiffness after prolonged standing. 10 slow repetitions, morning and evening.
- Standing Hip Hinge (Wall Drill) - Teaches neutral pelvis and spine positioning while upright - directly retrains posture in the standing position. 10 reps, 2 sets.
- Calf Raise + Weight Shift - Improves circulation and reduces lumbar fatigue during unavoidable prolonged standing. 20 slow reps.
💡 Soft CTA: Not sure which of these applies to your pattern? Backed AI identifies your specific posture type first - then builds a corrective plan that targets the actual source of your pain, not just the symptom.
Step-by-Step Recovery Framework: Lower Back Pain from Standing
Physiotherapists often recommend a structured progression rather than random exercises. Here's an effective three-phase approach:
Phase 1 - Decompress and Release (Days 1-7) Goal: Reduce accumulated tension and restore basic mobility.
- Morning: Cat-cow x 10, child's pose 30 seconds
- Evening: Hip flexor stretch, knee-to-chest hold
- Avoid prolonged standing until pain is below a 4/10
Phase 2 - Activate and Strengthen (Weeks 2-4) Goal: Build the muscular support that takes load off the lumbar spine.
- Daily: Glute bridges, dead bug, bird-dog
- Add: Standing hip hinge wall drill for postural retraining
- Start with 2 sets, build to 3 sets over the week
Phase 3 - Load and Integrate (Weeks 4-8) Goal: Make corrected posture automatic during standing activities.
- Add: Calf raise and weight shift drills during standing tasks
- Practice: 5-minute standing posture checks using a mirror or phone camera
- Build standing endurance gradually - add 5-10 minutes of comfortable standing daily

How to Stand Longer Without Lower Back Pain
Beyond exercises, how you stand matters significantly.
- 👟 Wear supportive footwear. Unsupportive shoes change how load travels up the kinetic chain. A neutral, cushioned shoe redistributes pressure far more evenly.
- 🦶 Use an anti-fatigue mat. Standing on a slightly padded surface reduces lumbar compression during unavoidable prolonged standing.
- 🔄 Shift your weight regularly. Moving from foot to foot every few minutes prevents any single muscle group from fatiguing. Even subtle micro-movements help.
- 🪑 Use the one-foot-up position. Resting one foot on a low stool (around 6 inches) for intervals while standing significantly reduces lumbar curve and muscle tension.
- 📏 Check your screen height. If your screen or work surface is too low, you're likely leaning forward - which compounds the lumbar load while standing.
Research & Expert Insight
Research in musculoskeletal health consistently confirms that postural alignment is the primary modifiable factor in standing-related lower back pain. Studies in occupational health found that workers who receive postural correction training and core strengthening programs report substantially lower rates of standing-related lumbar pain compared to those who only receive ergonomic equipment changes.
Posture specialists note that the glutes are often called the "forgotten muscle" in lower back pain treatment. When the glutes are chronically underactive - which is almost universal in desk workers - the lumbar erectors compensate. This creates a predictable cycle: the longer you stand, the faster the lower back fatigues, because it's doing the work of two muscle groups.
Research also confirms that correction of anterior pelvic tilt through targeted hip flexor release and glute activation is one of the highest-impact interventions for relieving standing-related lumbar pain in otherwise healthy adults.
When This Approach Doesn't Work
Targeted exercises and posture correction work for the majority of cases. But certain situations require medical evaluation:
- Pain that radiates down the leg - sciatica, disc herniation, or spinal stenosis may be present
- Pain that doesn't improve at all with position changes - could indicate a non-mechanical cause
- Neurological symptoms - numbness, tingling, or weakness in the legs warrants urgent assessment
- Pain after recent spinal surgery or injury - a physiotherapist or specialist should guide your recovery
- No improvement after 6-8 weeks of consistent, correct exercises - a full physiotherapy assessment is warranted
This guide is designed for postural and muscular standing back pain - the most common type. Always see a healthcare professional if you're unsure about your symptoms.
Final Takeaway
Lower back pain when standing is one of the most common - and most correctable - postural complaints. The fix isn't rest, it's targeted activation. Strengthen the glutes and core. Release the hip flexors. Retrain your standing posture. And build the endurance gradually over 6-8 weeks. Most people who address the actual cause rather than the symptom see meaningful improvement within a month.
Why Most Exercise Plans for Standing Back Pain Fail
Millions of people search for "lower back pain stretches" and find the same list. Hip flexor stretch, child's pose, knee hug. They feel better for a day. The pain comes back next time they stand at the kitchen counter for 20 minutes.
Here's what's going wrong:
- Stretching without strengthening - releasing tight muscles without activating weak ones doesn't hold. The same pattern returns within hours.
- No diagnosis of the actual pattern - anterior pelvic tilt, flat back, and muscle fatigue all cause standing back pain, but they each need different exercises. Doing the wrong ones can make things worse.
- No progression - the same routine done at the same difficulty stops creating change after week two. Without progression, there's no long-term improvement.
- No feedback loop - most people have no idea if their posture is actually improving between sessions. Without tracking, regression goes unnoticed until the pain returns.
A Smarter Starting Point 📱
Backed AI was built for exactly this kind of problem.
Using your phone's camera, Backed AI scans your posture and identifies your specific pattern - whether that's anterior pelvic tilt, flat back, rounded shoulders, or something else entirely. From there, it builds a fully personalised exercise program targeting the real source of your standing pain.
What makes it different:
- 🎯 AI posture analysis - identifies your specific postural driver before any exercises begin
- 📈 Progressive programming - adjusts week by week so you're always creating positive change
- ⏰ Daily habit reminders - keeps you consistent beyond the first 3 days
You don't have to keep guessing what's causing your lower back pain when you stand. The answer is in your posture pattern.
Download Backed AI and start correcting your posture today.
FAQ
Q1: Why does my lower back hurt when I stand but not when I sit?
Standing increases compressive load on the lumbar spine and demands continuous muscle activation. Sitting shifts the load and reduces demand on the lower back extensors. If standing triggers pain and sitting relieves it, the likely cause is postural misalignment or insufficient posterior chain strength - both correctable with targeted exercises.
Q2: How long is too long to stand without a break?
Posture specialists suggest taking a short movement break every 30-45 minutes of continuous standing. Research shows that even a brief walk or position change significantly reduces lumbar muscle fatigue and cumulative disc pressure.
Q3: Can weak glutes cause lower back pain when standing?
Yes - and this is one of the most common overlooked causes. When the glutes are underactive, the lower back muscles compensate and fatigue far more quickly during standing. Glute strengthening exercises like bridges and hip hinges are often the most effective single intervention.
Q4: Is standing worse for the lower back than sitting?
Both can cause lower back pain when done with poor posture or for extended periods. The key difference is that standing back pain tends to be muscular and postural, while sitting back pain often involves disc compression. Both respond well to corrective posture and strengthening work.
Q5: When should I see a doctor for lower back pain when standing?
See a doctor if your pain radiates down the leg, is accompanied by numbness or tingling, has not improved after 6-8 weeks of appropriate exercise, or developed after an injury. These symptoms may indicate a disc, nerve, or structural issue that requires professional assessment.


